What Is Colorectal Cancer?
Colorectal cancer includes two types of cancers: cancer of the colon (large intestine or bowel) referred to as colon cancer, and cancer of the rectum (the end portion of the large intestine) or rectal cancer. Both types of cancer have many features in common, so they are collectively called colorectal cancer. The colon and the rectum form part of the digestive tract, also called the gastrointestinal or GI tract.
The Colon’s Main Functions
Re-absorb water and some nutrients such as the salts sodium, potassium and chloride from what we eat
Formation and compaction of waste
Fermentation of some indigestible food matter by beneficial bacteria
Generally, colorectal cancer spreads fairly slowly, more slowly than some other cancers. It can stay in the colon or rectum for months or years, and, if it is not treated, can spread to other parts of the body. If caught in the early stages, colorectal cancer is often curable.
Most colorectal cancers evolve from small mushroom-like growths known as polyps. Sometimes the polyps can be flat, making them harder to detect. While most polyps are benign (non-cancerous), as they evolve they may become cancerous.
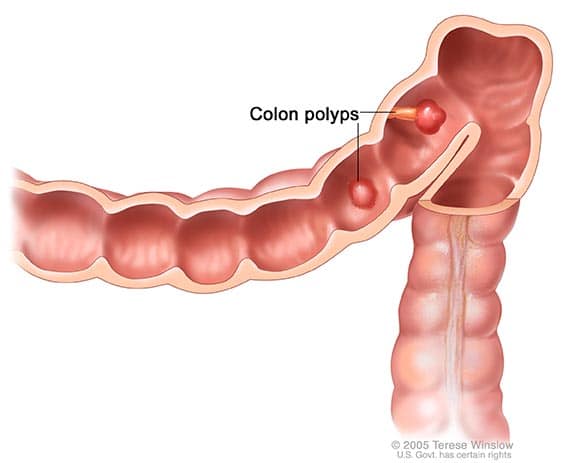
Over time, the benign polyp may grow through some or all of the tissue layers that make up the colon and rectum and become malignant, invading nearby tissues and structures. Eventually, malignant tumour cells can reach the blood and lymphatic system and travel to other parts of the body such as the liver or lungs, causing cancer to develop in these organs. The spread of the cancer to another organ is called metastasis.
Keeping up to date with colorectal cancer screening is an important part of prevention. A screening test checks for the presence of colorectal cancer when there are no signs and symptoms of the disease. Participating in screening helps to remove precancerous polyps before they become cancerous and helps to detect colorectal cancer at an earlier stage, when the cancer is more treatable.
Early-stage disease can present very minor colorectal cancer symptoms, sometimes presenting no symptoms at all. This underlines the importance of keeping up to date with screening.
Common signs and symptoms of colorectal cancer

Many of these signs may also be caused by other gastrointestinal conditions, such as Crohn’s disease, ulcers or hemorrhoids, but they should always be discussed with your doctor to receive the correct diagnosis. If you are experiencing any signs or symptoms of colorectal cancer, be sure to talk to your doctor without delay.
Certain lifestyle factors may also contribute to an increased risk of developing colorectal cancer
UNDERSTAND YOUR GENETIC RISK
Genetic testing can provide crucial insights into your risk for colorectal cancer. By identifying inherited syndromes and mutations, you can take proactive measures in prevention and early detection. If there is a history of colorectal cancer in your family, consider discussing genetic testing with your doctor.
Take Charge of Your Health
Regular screening is crucial for early detection of colorectal cancer. By staying up to date with screenings, you can catch potential issues early, when colorectal cancer treatment is most successful.